A new standard for insurance collections
Amperos uses agentic AI to recover insurance revenue end-to-end — driving more collections, faster.
Amperos uses agentic AI to recover insurance revenue end-to-end — driving more collections, faster.
Trusted by leading healthcare providers and RCM teams














End-to-end insurance recovery
Amperos manages to full insurance collections process, from follow-up to complex denials.
First-touch automation
Empower your team to focus on higher-value works by assigning Amperos to first-touch denials, resubmission, and more.
Complex denial resolution
Our combination of AI optimization and a team of tenured revenue cycle specialists drives superior recovery on the most complex claims.
Configurable workflows
Your Amperos deployment team maps your exact workflows, payor priorities, and SOPs into the system. You define the rules. We configure them.
Higher claim recovery compared to traditional vendors
Reduction in AR backlog
Lower cost to collect
Claims processed across leading healthcare providers
Higher claim recovery compared to traditional vendors

Identify and pursue high-value claims that traditional workflows leave untouched.

Keep things moving with prioritized workqueues and automated follow-ups.

Reduce the operational burden of repetitive collections work through automation.

Track activity, progress, and outcomes across your entire claims pipeline.

Less time spent chasing outstanding claims means more time growing your practice.

"Boulder Care is expanding rapidly to reach more patients who are in critical need. The reality is that we need to adapt our operations for scale in the modern age"
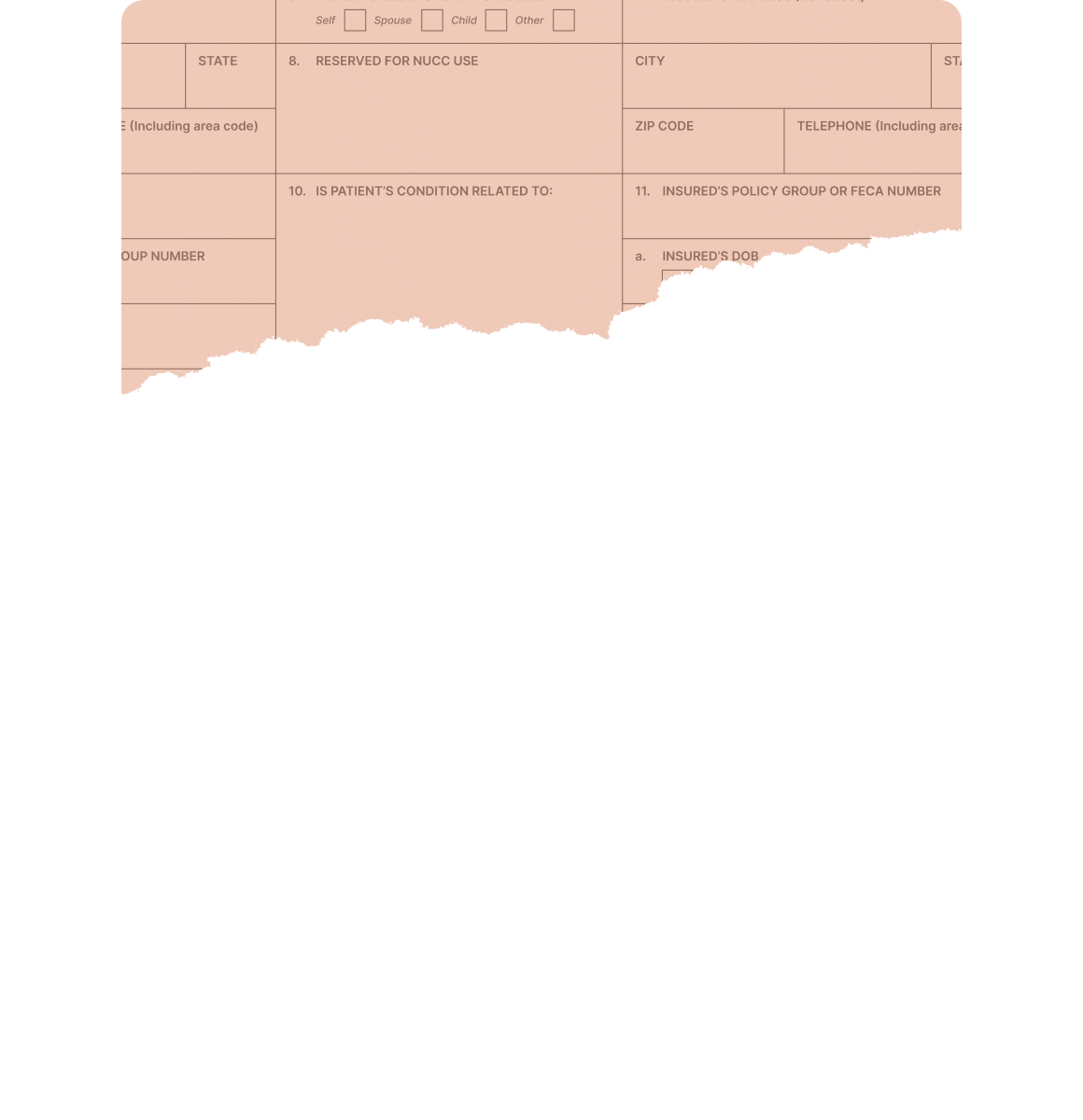






AI agents work claims end-to-end, while Amperos RCM experts provide oversight and guidance for resolving complex denials and escalations.




AI agents work claims end-to-end, while Amperos RCM experts provide oversight and guidance for resolving complex denials and escalations.



Every interaction, update, and decision is captured and summarized so teams always know the status of their collections activity.




Workflows run reliably across claims, reducing the operational variability that often slows collections — whether following your existing SOPs or proven best-practice workflows.



Claims aren’t just worked. They’re pursued through to outcome, with clear accountability for results.
Integrate Amperos with your existing practice management and EHR systems.
Analytics identify patterns across payors, denials, and workflows to help teams uncover root causes, improve processes, and recover more revenue.


Claims are automatically categorized and prioritized so the highest-impact work gets attention first.

Amperos connects claims, payor interactions, and collections activity into a single system

eClinicalWorks

Athenahealth

NextGen

Epic

ModMed

Imagine

Dentrix